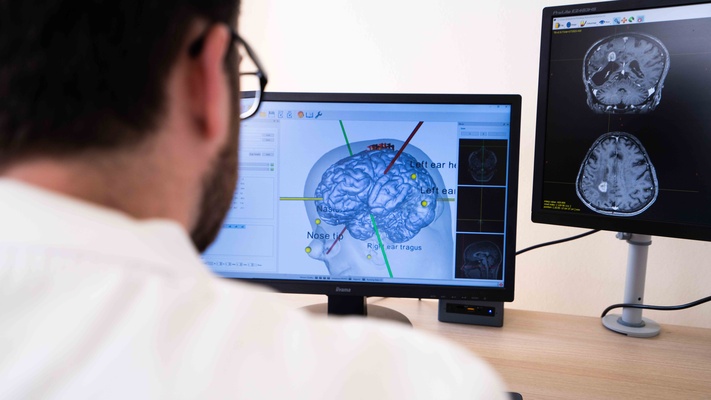
Planning glioma resection with MRI-guided neuronavigated Transcranial Magnetic Stimulation
The majority of malignant brain tumors are glioma’s classified in low-grade ( I and II) or high-grade ( III and IV) (Stieber, 2001). The approximate average survival time for patients with low-grade gliomas is 7 years, where the survival time decreases rapidly for patients with grade III and grade IV gliomas (Claus et al., 2016). Optimal extent of resection (EOR) directly correlates with the survival rate of glioma patients, therefore gross total resection (GTR) should always be the goal of neurosurgical procedures (Krieg et al., 2015).
A multimodal approach of preoperative mapping and intraoperative mapping is often needed to differentiate between healthy brain tissue and malignant tissue. Direct Electrical Stimulation (DES or DCS) is the current golden standard for differentiation. However, DES is an invasive technique with many disadvantages like large exposure area of the cortex . Furthermore, DES prolongs the duration of the surgery and leads to stressful situations for the patient as awake stimulation is needed to observe the brain areas involved in functional responses (Paiva, Fonoff, Marcolin, Cabrera, & Teixeira, 2012).
With MRI-guided neuronavigated Transcranial Magnetic Stimulation (nTMS) the motor cortex can quickly and accurately be mapped prior to glioma resection surgery. By registering the exact location of the TMS coil with respect to the brain and the physiological response that is induced by that pulse, functional, healthy brain tissue can be differentiated from unhealthy, dysfunctional glioma tissue. This data can help neurosurgeons in planning the operation upfront and to clinical added value for the patients because the procedure is non-invasive
Studies regarding the application of nTMS in presurgical planning have shown that nTMS presurgical planning results in less residual tumor tissue in the brain after resection. Additionally, a smaller craniotomy and a decrease in new functional deficits have been reported with presurgical planning with TMS